Tag: Andrew Doody
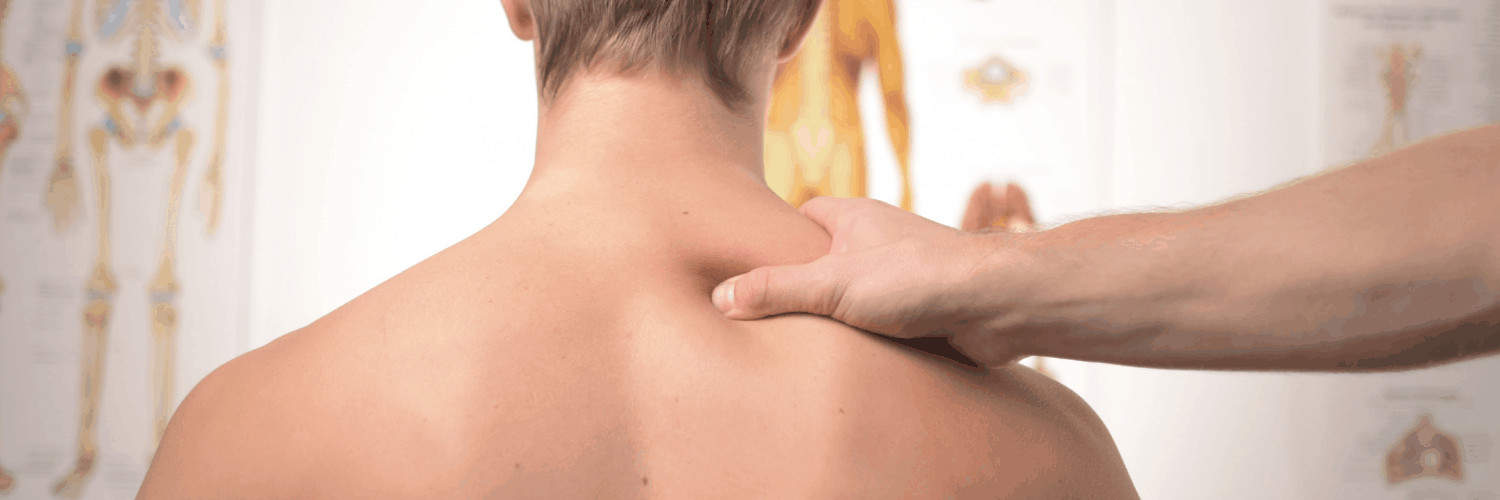
Much like getting fit, improving posture is a long term game. Trying to stand or sit up straight when you remember isn’t really going to cut it. First of all, you obviously forget, but secondly, using those big mobility muscles to pull you upright causes them to tire quickly and build up lactic acid, at which point you slump for quick comfort.Many things can be causing bad posture and pain, so it’s worth getting it assessed first. Even if there’s no major problems but it’s been happening for a while, some mobilisation, adjustment and tailored exercises may well be needed.To help posture long term we need to do two things:
Change the habits encouraging bad posture, and get the right muscles to do the job.
Try to identify when posture is bad. If it’s sitting at a desk/computer, get the desk assessed and altered. If it is slouching on the sofa, sit upright, bottom to the back of the seat, maybe a cushion in the small of the back, feet on the floor. Be aware of looking at phones for too long. Read my full blog here on how to set up your workstation properly. Using and strengthening correct muscles to hold your posture is equally important. The postural muscles are designed to hold you in a better position with less effort for much longer without tiring. If you are nicely upright and relaxed your head is largely balanced on top of your spine. Just a little angle forward (to look at your phone for instance) or slumping, and suddenly it takes a huge muscle effort to hold it up. To get these postural muscles working and strengthened can be a little tricky at first as you try to co-ordinate them. I often suggest something like Pilates or the Alexander Technique, but even just doing more core stability exercises in the gym or at home will help.
Osteopathy can treat a vast array of joints and musculoskeletal issues of the body caused by poor posture, including:
- Non-traumatic back pain including lumbago and sciatica pain management
- Stress-related musculoskeletal problems
- Neck pain & headaches including migraine prevention
- Pregnancy-related musculoskeletal problem
- Postural-related problems including shoulder, hip, knee and/ or ankle pain
- Workstation-related problems
- Restricted Mobility
If you’d like to understand the underlying causes of your pain and discomfort and a personalised treatment plan for recovery, book an osteopathy appointment.
___________________________________
OSTEOPATHY AT FLEET STREET CLINIC
Andrew Doody is an osteopath at Fleet Street Clinic and is fully registered with the General Osteopathic Council (GOSC).
Book an appointment with him if you have any musculoskeletal injuries by calling +44 20 7353 5678, email info@fleetstreetclinic.com or book an appointment online.
Stress, everyone has it too some degree – some is healthy, lots is not.
What effect does a lot of stress have on your body?
Stress is known to affect the whole body but we shall focus on the way it affects the neck and shoulder girdle. Much research over the years has confirmed a connection between neck pain and stress. One study, for instance, in the BMC Musculoskeletal Disorders Journal, found that of nearly 500 people tested, those with stress, anxiety or depression had significantly worse neck pain that lasted longer than those without.
Even without the research though, lots of people will tell you that stress makes their neck and shoulders feel tight. When someone consciously relaxes, one of the most noticeable things to happen is their shoulders drop a couple of inches.
I’d go even further, and say that as the brain recognises the connection between stress and neck & shoulder tightness (and in fact initiates it). Let me explain, if someone has a tight neck or shoulders due to another cause, the brain, rightfully or wrongfully interprets this as the body being stressed.
If you have those muscles massaged and loosened and the neck releases, most people feel immediately less stressed.
Some of the many causes of neck or shoulder girdle dysfunction and stress crossover, such as long hours working at a computer to meet deadlines, and not sleeping very well. From this, secondary symptoms can develop, most commonly, headaches.
Some exercises that I recommend for tension headaches can be found here.
So what can we do about it?
Well, as always, firstly make sure there is nothing else causing your symptoms. Get a health professional to assess you and diagnose what is causing your symptoms.
If the diagnosis is stress or posture-related then get it treated. It’s important to treat from both a musculoskeletal point-of-view as well as understand and address the cause of your stress.
Alongside this, there are a number of at-home techniques you can do to help ease the tension in your neck and shoulders.
1. Do neck and shoulder mobility exercises.
A couple of quick and easy exercises I would recommend would be:
Exercise 1 :
https://www.youtube.com/shorts/vSBsfMnMx6M
Exercise 2 :
https://www.youtube.com/shorts/X6XJdciru0Q
Exercise 3 :
https://www.youtube.com/watch?v=A0HWan_RPwo
2. Get a good amount of quality sleep.
Stress is known to affect your ability to sleep. There are things you can do to give yourself the best chance of sleep.
– Make sure you’re comfortable in bed
– Be strict with no blue light (screens) for at least an hour before bed
– Having a warm bath or shower to help you relax
3. Find something to relax you.
It doesn’t have to be meditation or yoga, it could be exercise or playing an instrument. Perhaps avoiding instruments such as the violin which will exacerbate neck & shoulder pain. The ides if to find something that sends you to your flow state. Something that will distract you that you really enjoy and will relax you.
4. Work in a good environment.
Set up your workstation in an ergonomic way will do wonders for your posture. Remember to have lots of breaks and consider investing in a standing desk. If you’re interested in knowing what an ergonomic workstation set up looks like, continue reading here.
5. Speak to a healthcare professional.
Your health professional may recommend you get support or therapy for your stress, anxiety or depression, or any mental health issues you may be experiencing.
_____________________
Is Osteopathy the right path for you?
Osteopathy is a holistic way to diagnose and alleviate stress-related musculoskeletal problems including shoulder and neck pain and secondary symptoms such as headaches. The treatment is catered to the individual and Andrew will take all aspects of a patient’s lifestyle into consideration when suggesting a treatment plan.
All treatment starts with an initial consultation followed by any recommended follow up treatment. You can book your initial consultation with Andrew Doody online.
A good night’s sleep is essential to your health, and an important part of your overall well-being. People spend about a third of their lives in bed, so it’s vitally important to get it right when it comes to back health. Back pain can significantly affect a person’s ability to get the quality and amount of sleep they need. Furthermore, poor bed posture can worsen or even be the cause of backache in the first place. This is because certain positions can place unnecessary pressure on the neck, hips, and back.
This blog will provide an in-depth review of different sleeping positions and types of beds and the impact both have on your quality of sleep.
Sleeping positions
Before looking at the positions to sleep better, it is important to address a few crucial things. First and foremost, you should be comfortable. For a good night’s sleep, waking up feeling properly rested and not in pain is the most important thing. If any of these positions cause issues, don’t hesitate in letting me (or another osteopath) know so that alternative suggestions can be made and you find something else that works for you.
Secondly, I know it’s not always possible to control what position you get into once you’ve fallen asleep. However, this is where perseverance comes in, if you keep trying, your body can adapt in a week or two. Pillows are always a good ally, to stop you rolling one way or the other.
Here are some positional tips that can help you get a better night’s sleep:
1. The Classic: Lying on your back.
Lying on the back is probably the best all-around sleeping position for a healthy back. It ensures good spinal alignment from the head and cervical vertebrae, through the thoracic and lumbar, all the way down to the pelvis. Because the back is the body’s largest area, weight is most widely distributed in this position, minimising pressure hot spots. This doesn’t suit everyone though, some people don’t feel as ‘nested’ as in other positions so, they struggle to get to sleep on their backs. Also, snorers may find that this position exacerbates the problem.
For people who like back sleeping, it’s definitely worth adding a pillow under your knees. It loosens the hamstrings a little and takes some pressure off the lumbar lordosis.
2. The Foetal Position: Lying on your side with your knees up a little.
This is a fairly intuitive position to get into if you have lumbar disc issues as it slightly flexes the low back and opens up the gaps in the facet joints.
Again, a good tip in this position is to use a pillow, however, this time put it in between your knees. This stops your top leg dropping forward and rotating the low back. It also aligns your hips and pelvis better, and feels more comfortable on the upper knee.
Try to swap sides from time to time if you’re lying in the foetal position.
3. Face Down: Lying on your stomach.
I normally ask people to avoid this position, it’s usually quite problematic for the neck as well as the low back. Unfortunately, for a lot of people, it’s the only position they can fall asleep in, or any other position makes them snore. If you’re one of them, reach for that extra pillow again and put it under your low stomach and upper pelvis to take the pressure off the low back. This is a good idea if you’re having a massage too. Front lying needs a much flatter pillow (or even no pillow) under the head too.
If you’re someone who falls asleep on their back or side, then rolls over in their sleep and wakes up on their stomach, try hugging a large pillow against your chest and stomach to keep you in position. Another reason sleeping on the front is considered bad is because the head is usually turned to one side. This twists the spine and places additional stress on the neck, shoulders, and back. To avoid this, you can try lying face down. Place a small firm pillow or tightly rolled-up towel under the forehead, or better still a face pillow, allowing room to breathe. In this position, you should still place a pillow under the stomach.
4. Reclined Sleeping.
If all else fails, you can try sleeping in a reclined position. People with spondylolisthesis, for instance, may resort to this after finding it comfortable falling asleep in a recliner chair. There are beds available that can be sat up slightly. So, this is worth investigating.
What about the perfect bed for sleep?
There are so many different opinions about beds that I don’t even know where to start, nonetheless here’s mine.
Spend some time and effort (and dare I say money) choosing a bed and mattress. People seem happy to spend thirty times or more on a car than a mattress, but remember, a third of your life is spent in bed!
It’s really difficult to choose a mattress on a twenty minute trip to the bed store, so really take your time, spend an afternoon there, take your shoes off, try different sleeping positions, not just lying on your back! Do your research before you go, but make sure the review sites you look at aren’t secretly run by a bed company, or affiliated to one.
Firmness
Try not to be seduced by softness. Lots of people jot down the name of a mattress they’ve found comfortable in a hotel, and while this can sometimes be a good indicator, you should know that hotels buy mattresses to give you a couple of nights feeling like you were sleeping on a cloud, but these mattresses are usually not supportive enough to be using full time, especially if you have low back issues, which can be aggravated over weeks and months. Often the mattress in a big hotel chain is not available to buy for the public as they are specifically manufactured for different hotels’ standards.
A fairly firm mattress is usually a good idea, perhaps with a shallow in-built topper. This can give you the support you need for your low back while the topper takes the pressure off bony prominences and allows shoulders and hips of side sleepers to sink in a little. I suggested a built in topper as they are usually better segmented and don’t allow stuffing to move around and bunch up as much. However, removable toppers give you more scope to adapt by removing it if needed, and also allow you to flip the mattress.
Mattresses that are fully stuffed as well as sprung are good and supportive. Price is a good indicator for a quality mattress. £1,500 for a king size mattress is not excessive. While we’re talking about price, beware of anything that seems too good to be true. The “Winning awards” mattresses need to be checked as to which award, and who’s giving it!
Memory Foam Mattress
Patients have different opinions about memory foam mattresses. While some patients swear by them, others do not get along with them. I’d like to reiterate the price, if you’re set on a memory foam mattress, find the one with better quality, so it doesn’t start to develop a permanent dip where you lie. It’s all about density which is measured in pounds of pressure per cubic square foot. More is normally more expensive and better quality, but at the same time is also more supportive and feels harder.
There can be a problem with memory foam mattresses feeling too hot. While many of the better brands have addressed this to an extent, many memory foam mattresses have become hybrids so, it’s not just 100% foam any more.
Platform Bases
Mattresses should be changed about every 8 years, but you can keep the same bed base, of course, as long as it’s not damaged. Divans have pretty thin wood tops that can crack or bow so, check it carefully.
In my opinion, a platform base is always the best. If the base is sprung, the whole mattress will start to fold which is usually not what they’re designed to do. A slatted base is slightly better than a fully sprung one, but still not as good as a solid base.
Pillows
Finally, I should mention pillows. Pillows are very subjective to the person, and especially to any neck/upper back/shoulder girdle conditions they may have.
As a rule of thumb (and this is painting with a very broad brush) people seem to usually have too much pillow depth more often than too little. One medium depth pillow is usually best if you don’t have any specific issues. I find feather works well as you can punch and mould it to the right height and shape, so there is some support under your neck but that’s very much a personal preference.
I rarely see anyone who gets on well with memory foam pillows (there are the odd one or two) or sprung pillows.
The price of a good feather pillow is probably about £50, but as I said right at the start, I want you to not only be in a good position, but also comfortable and pain-free during the night and the next day, so if a £5 pillow works for you then that’s absolutely fine. Don’t forget most pillows can be laundered regularly which may give (especially feather pillows) some of their volume back.
If you are experiencing neck pain though, get your neck examined and treated first and ask your osteopath what pillow they would suggest for you specifically going forward.
BE ‘BED FIT’
The healthier and stronger your back is, the better night’s sleep you will get and the better your back will be when you get up in the morning.
Core strengthening exercises will help support the back during the night and prevent back spasms. Gentle stretching before bed can increase flexibility and help to relax the body and reduce stress.
Take care getting in, and especially out, of bed. Take your time. When you wake up in the morning, allow a few minutes to get your muscles and joints moving fully instead of leaping out of bed at the alarm. Roll onto your side then use your arms to push you upright while your legs drop over the side, then sit there for a minute moving gently before slowly standing up.
Perhaps most importantly, if you do have a back or musculoskeletal issue, get it checked. A health professional can assess why you’re suffering and help treat the symptoms. They can suggest the correct investigations, treatment and exercises, as well as further helping you to choose that all important correct mattress.
Booking an appointment with an osteopath could be the start of ending your back pain for good!
Tension Headaches
80% of adults will experience tension headaches at some point. They are caused by tight muscles surrounding the neck, pressing on nerves that refer pain to another location, in this case, the head.
Most often, tension headaches are triggered by lifestyle factors such as poor posture i.e. from sitting hunched over at a computer and/or stress.
Almost all types of headache activate the same pain receptors so it can be difficult to know if your headache pain is a sign of something more serious. When experienced suddenly or regularly, you should always get your headache pain assessed by a health professional to rule out any serious health conditions.
Stretches
If you have been diagnosed with tension headaches alone, the good news is they respond well to treatment. Here are a few stretches to help relieve the pain they cause:
Stretch 1
This is a neck flexion stretch that you should repeat 10 times, holding for a few seconds each time.
https://www.youtube.com/watch?v=XZe7c0kpZA4
Stretch 2
This is a stretch for the upper trapezius that you should repeat 10 times, holding for a few seconds each time.
https://www.youtube.com/watch?v=yRtWVO1zKLE
Stretch 3
This is a stretch for the scalene muscles that you should repeat 10 times, holding for a few seconds each time.
https://www.youtube.com/watch?v=dUHsyB-opYg
Stretch 4
This is a levator scapulae stretch that you should repeat 10 times, holding for a few seconds each time.
https://www.youtube.com/watch?v=3k9cNIlIE-Q
For more information on Osteopathy services at Fleet Street Clinic.
You can book an initial consultation with Andrew Doody online.
How walking can help Chronic pain
Firstly, what is chronic pain?
Chronic or persistent pain can be explained as pain that carries on for longer than 12 weeks despite medication or treatment.
The root cause can vary person-to-person, with it sometimes due to illness or an injury. In other cases it can be due to being overweight, having years of poor posture or improper lifting of heavy weights. It can be debilitating but movement is known to help.
As an osteopath, the conversation I seem to have at least once-a-day is; how much exercise should someone who is in pain be doing?
As you can imagine every case is different, and exercise advice varies hugely from person to person and condition to condition. There is a big difference between chronic pain and recovery from injury pain. I am focusing on exercises for people with chronic pain conditions, specifically walking.
Many people with chronic pain are afraid that movement, including walking, will worsen pain. But as many have subsequently discovered, the opposite is very often true. Using your muscles and joints less can often cause pain to becomes worse. Gentle exercise like walking can really help to bring those pain levels down, as well as many other benefits like improving your circulation, strengthening your bones and of course helping to keep those extra pounds off.
Here are tips before you start:
1. Talk to your healthcare professional first
You should always take the advice of a health professional before starting any exercise. They can ensure it is safe for you to start, and guide you with the types of exercises you should begin with. They will also help you understand your limits and outline suitable goals. As a rule of thumb, if you are in pain, stop!
I, or another osteopath, can check your posture and gait and give you tips on engaging the correct muscles.
2. Get the right shoes
A good pair of supportive trainers will prove invaluable. Walking boots that protect the ankle are only really required if you’re planning to walk on loose surfaces or heading off into the mountains. Otherwise, walking trainers will suffice. To find out more about choosing the right footwear, read our blog on How To Avoid Running Injuries.
3. Start slow
What we’re aiming for is about half an hour to an hour of physical activity five days a week, but this may take some time to achieve. There’s no rush! A good indicator that you are at the right intensity level is that even though your heart rate is up a little, you are still able to carry on a conversation while walking. When starting your walk don’t go full speed immediately. Allow your muscles and joints to warm up for the first few minutes before getting up to speed. This will help prevent damage and injuries.
4. Keep hydrated
You may need to carry a bottle of water, especially for walking in hot weather. If the weather is hot, make sure you also take sunscreen and a hat to stop sunburn.
5. Finally, try to enjoy it!
The more you enjoy it, the easier it becomes. Find somewhere nice to walk, even if that means
driving somewhere. Listen to music/ podcasts/ audiobooks, or even better get a walking buddy to join you for a chit chat along the route.
For more information on osteopathy services, visit the main page.
___________________________________
OSTEOPATHY AT FLEET STREET CLINIC
Andrew Doody is an osteopath at Fleet Street Clinic and is fully registered with the General Osteopathic Council (GOSC).
Book an appointment with him if you have any musculoskeletal injuries by calling +44 20 7353 5678, email info@fleetstreetclinic.com or book an appointment online.
With (hopefully!) sunnier and longer days upon us, summer is a great time of year to get your running shoes on. As a keen runner myself, I understand the appeal; it’s pure, it’s meditative, and it gets your blood pumping like little else.
Unfortunately, for all its positives, running can be problematic for the body and it tends to bring out minor issues and turn them into major ones. These often include achilles tendonitis, shin splints, plantar fasciitis, ITB syndrome, stress fractures, hip and lower back issues, and more knee problems than I have time to list.
Many of the problems from running come from two areas. Firstly, heel strike which is where the heel hits the ground repeatedly and sends a shock through the whole skeleton which causes issues from the heel itself all the way up to the lower back. Secondly, gait – which is the way a person walks; the whole lower limb (especially the knee) is quite finely tuned to work in certain ways, and anything that affects that can begin to cause problems. A dropped arch, tight muscle, old injury, slight one-sidedness etc can bring these issues on.
What can be done to prevent these issues?
Like always, the number one rule is to get any symptoms you are experiencing looked at as soon as possible. Early diagnosis, advice and treatment is vital.
One thing that can really help heel strike and gait is by getting the right trainers. Here’s a few things to consider:
- Don’t confuse fashion and effectiveness. Good running trainers generally don’t look cool! Some of the bigger brands will advertise to you that they are great for sports but do your research. I would usually recommend Asics or Brooks.
- Replace your shoes regularly. The soles of most trainers are good for about 200-250 miles maximum. So, if you’re running 20 miles per week, you’ll probably need to replace them after 4-6 months.
The shoe may still look okay after that but there is an increased risk of injury. It is, therefore, important to ensure that you are replacing your trainers as regularly as required. - You don’t need to buy the most recent model. Many of the best running trainers are on their 20th/30th or so iteration. When a new model is released the price of the last couple of iterations will drop quite significantly, and will still be an excellent option.
- Good arch support. Trainers largely work on preventing pronation etc. by the way they flex. Many have little if any arch support, even with good ones you may need an additional orthotic insole made for your specific needs. This may also mean you need half a size bigger.
- Speak to the experts. A running machine in a shoe shop is useful, but remember the shop assistant has probably only had a brief introduction in what to look for, and no idea of your other contributing factors. Speak to a specialist – an osteopath, podiatrist, or physio.
_____________
OSTEOPATH AT FLEET STREET CLINIC
Andrew Doody is an osteopath at Fleet Street Clinic and is fully registered with the General Osteopathic Council (GOSC).
Book an appointment with him if you have any musculoskeletal injuries by calling +44 20 7353 5678, email info@fleetstreetclinic.com or book an appointment online.
SUMMER CYCLING
Summer is the perfect opportunity to dust off your bike and think about turning that commute into an opportunity to get fitter or shed a few pounds!
Cycling – a low impact sport
Compared to many sports, cycling is one with a relatively low injury rate. Crashes and collisions apart, cycling is impact free – good for your joints and muscles. In addition, if you select the correct gear to match the terrain, it means that you can avoid overloading your muscles and joints, keeping the cranks spinning rather than pushing a big gear.
Also important is that because your feet are fixed in place, spinning the cranks requires very little coordination, which also reduces the risk of injury due to poor technique, which is very common while running. Still, despite all these advantages, cyclists can, and regularly do, suffer overuse injuries.
Fix a good riding position:
One of the main issues is the set up of the bike itself. Here are a few pointers as to how to best achieve a good riding position:
SADDLE HEIGHT
This should be positioned so that when the pedal is at the bottom of the stroke and the ball of your foot is on the pedal, your knee should have a slight bend in it. If you want to get technical, saddle to pedal distance should be 109% of your inside leg measurement. Hips shouldn’t move sideways during crank rotation and you shouldn’t have to stretch at the bottom of the pedal stroke. Don’t be put off by feeling you have to come off the saddle to touch the floor.
SADDLE ANGLE
This should be in a horizontal position, parallel with the floor when viewed side on (but sometimes a very slight downwards tilt can be helpful for those who experience a lot of pressure in the perineum area. However, don’t do this just because it feels more comfortable, as this can cause lessen support and affect riding position).
POSITION OF THE SADDLE
With the pedals adjusted so that they are at the three o’clock and nine o’clock positions, a vertical line dropped from the kneecap of the forward knee should pass through the axle of the pedal.
HANDLEBAR POSITION
This is where opinion varies a little. Racers want the handlebars low to lower wind resistance, climbers want the handlebars low so they don’t feel too high when the bike’s angled up. The rest of us want them higher than this. A good rule of thumb is that you don’t want to be leaning on the handlebars too much, only holding them. If it feels like your upper bodyweight is being supported by the handlebars, try them up a little. Not all bikes are adjustable enough at the front but a stem raise is a cheap efficient way of remedying this. A bit more height in traffic is safer anyway.
And if you haven’t bought your bike yet, put a bit of research into what frame/wheel size you need before you do.
Cycling is a great way to get fit and works well with core stability, however, if any injuries do niggle don’t push through and do get them checked out!
Osteopath at Fleet Street Clinic
Andrew Doody is an osteopath at Fleet Street Clinic and is fully registered with the General Osteopathic Council (GOSC).
For more information on our osteopathy services, click here.
Book an appointment with him if you have any musculoskeletal injuries by calling on +44 20 7353 5678 , email info@fleetstreetclinic.com or book an appointment online.
Osteopathic manipulation, or HVT (high-velocity thrust) as it is more technically known, is the “click” that many people associate with osteopathic treatment.
It is by no means always used by an osteopath, but when it is, it can prove to be a quick, efficient, and pain-free way of restoring function to a joint.
Many patients’ conditions may not be suitable for HVT, and many may not be keen to have it done anyway. In these cases, the osteopath will treat with a whole collection of other highly effective ways. HVT should be seen as a useful tool in some circumstances, but not a be-all and end-all of osteopathy.
So how does it work?
HVT is placing a short sharp tug though a joint, most often a spinal facet (which is what we will concentrate on here), a click may or may not be heard. The noise itself is a bit of a by-product. What it is has been disputed a little but the generally accepted explanation is that when the joint is stretched, the synovial fluid inside the joint itself physically does not stretch, so gas is forced out of solution causing gas bubbles that allow the joint to gap slightly, causing the clicking noise. This also explains why another click cannot be produced for a little while until the gas has been reabsorbed.
The gapping of the joint is the key to the effectiveness of HVT.
What I must point out at this point though is that the click is not a relocation of a joint.
Barely a day goes past that someone doesn’t tell me their osteopath “clicked something back in” often assuming it was a disc. As much as it can feel miraculous like this sometimes, and a patient can often feel and be quite a bit straighter following treatment, the HVT is about restoring function to the joint, not putting it back in place. Discs especially do not just “pop back in”.
So what does the gapping achieve?
Well, here we have to get a little technical. There are three predominant effects caused by HVT as far as we can tell.
Firstly, post-contractile sensory discharge or PCSD.
Imagine that the brain keeps many muscles at a gentle tension, this allows you to hold your posture. When an area is identified as problematic (painful or inflamed etc), the brain may choose to cause the muscles around the area to spasm, often to protect the area. The spasm itself may cause further pain. This then becomes a vicious circle and dysfunction.
Tension in the muscles is controlled by spindle fibres. This is what detects the short sharp tug of the muscles in HVT. Imagine the short sharp tug as a reset for these fibres. The brain then has to determine the level of muscle tension required and often can reset to the original tension, immediately bringing the joint out of spasm.
Massage of muscles, slow stretching over a longer period, has a similar effect but unfortunately can’t be performed on the small, deep muscles directly around and holding the joint.
Secondly, pain gate theory.
Even when nerves are reporting pain in a certain area, it is important that the body can still detect a soft touch in the same area. To achieve this soft touch and position detecting nerves override deep pain detecting ones. Where you ever told to rub your knee or elbow after you bumped it and it hurt? That’s pain gate, the soft-touch overrides the deep pain. It won’t stop it completely of course but even a little relief will make it feel better. In turn, this may again stop the brain causing the area to spasm.
HVT moves the joint quickly and sharply. This causes the positional detectors to immediately report this to the brain, inhibiting the deep pain.
Thirdly, meniscoid theory.
In a joint, smooth cartilaginous surfaces rub together, but they may not be quite as smooth as we used to think. Small pieces of cartilage appear to be in the joint. Possibly to fill small gaps; craters on a moonscape is a good way to think of it. It has been suggested that when the joint spasms, these small bits of cartilage, which are attached to the capsule around the joint can become trapped out of place. Gapping the joint allows the tethers to the capsule to quickly pull them back into place.
It’s possibly worth pointing out before I finish, that although I said earlier that the click is an unnecessary by-product, I do wonder if it could be argued that the psychological effect of hearing the click could be put forward as a fourth effect. Hearing a click and knowing that it may have relieved a painful joint does often make a patient immediately relax. This may itself be part of the healing process.
Osteopathic manipulation is often a quick efficient way of relieving dysfunction of a joint. It is not a miracle cure. Many other things have to be taken into account for the osteopath to treat fully and effectively.
HVT will not immediately heal damaged tissue or disperse inflammation, but it often is a good way to kick start the process.
Book an osteopathy appointment
By Andrew Doody | Osteopath | August 2019
So you’re back to work and the tree’s on its way back to the loft. Time to come through on all the New Year’s resolution bravado. Here are a few tips about how to do just that.
Create a plan
Decide what it is you’re wanting to achieve and tailor your program towards it. Do you want to lose weight? Get fitter? Tone up? All three? Don’t just choose the new fitness regime trend, think what you enjoy to do and go with that! You stand much more chance of continuing if you do. Identify times of day when you can exercise and which days you will do it. It’s much harder to stick to a regime that is just squeezed in when and if you have the time (not to mention inclination!)
Determine your readiness
Make sure you are mentally and physically ready to start, and more importantly ready to stick to, a regime. Check with your GP if you have any concerns about your health before you start. A good proportion of my new patients come from people who have caused injuries in the first few weeks, or even days sometimes, of starting a new regime. If you have any niggles, get them treated, and get advice on how to prevent them from recurring.
Be realistic
Set goals that are achievable and realistic. To lose a stone or be able to run 10k by Easter are realistic. To decide you are going to the gym every day before breakfast probably won’t last long. Fitness needs to be built gradually with a good base. Get advice on what exercise you need to do. Just running will help cardiovascular fitness somewhat, but needs to be part of a balanced all-around program if you want to be healthier generally. To maintain it, alone, running will also soon start to cause musculoskeletal problems.
Talk a friend into joining you
There will probably be no shortage of people thinking along the same lines as you. Teaming up hugely increases the chances of you both sticking to a program and makes it much more fun and less painful than trying alone. Even just planning together and talking about what you’re doing, (even if diaries don’t allow actually exercising together), is really encouraging.
Think long-term
Don’t look at this as a quick fix just to drop a few pounds. Take it easy and don’t rush. Tailor your plan around becoming more fit and healthy permanently. If you do it will help with so many other things, from energy levels to less aching joints or back, to stress relief and better sleep.
By Andrew Doody | Osteopath
Andrew is available for pre-exercise assessment, advice on exercise/regime planning, and diagnosis/treatment of outstanding or new issues, as well as advice on injury prevention. You can book an osteopathy appointment online.
As it’s backcare awareness week, let’s talk about back pain at work.
Back pain can be the result of heavy lifting, repetitive movement or simply by sitting at your desk all day.
We know how hard it is to live and work in pain and back pain is no exception. By now I’m sure we all realise that sitting for long periods is bad for you. But just how bad have our habits become? And what can be done about it?
Sitting in an office chair for long periods of time can wreak havoc on your lower back. In addition to many other joints and muscles. Simply stated, our bodies weren’t made to sit for prolonged periods of time. In fact, our bodies developed a heck of a long time before chairs were around at all.
According to research, the average office worker spends an average of 5 hours and 41 minutes per day sitting at their desk. The same study also found that those who sit longer at work are more likely to sit more outside of work as well.
Overall, sedentary jobs have increased 83% since 1950. With physically active jobs now only make up about 25% of the workforce. That’s 50% less than in 1950. Additionally, the average working week is longer. We now work an average of 47 hours a week, 164 more hours a year than 20 years ago.
On top of the time spent sitting in the workplace, on average, we spend 7 hours sleeping and 4.5 hours watching tv a day.
So should we be standing?
A recent study in the European Journal of Preventive Cardiology found that standing for almost six hours a day instead of sitting not only prevents weight gain — it can help people shed pounds.
They calculated that standing burned 0.15 calories more per minute compared to sitting. If an average person stood for six hours a day instead of sitting, they would burn an extra 54 calories a day. Some studies had it even higher.
In addition, muscle activity from standing is also associated with lower risks for strokes and heart attacks. Quite a few studies have shown that a single day of breaking up sitting with standing or short walks seems to have a beneficial effect on health parameters. Which include blood sugar control, blood pressure, and feelings of pain and fatigue.
However, before we all decide to stand all day instead, let’s look at the downsides. There’s a confusing array of conclusions from recent studies involving the health implications of standing vs sitting for long amounts of time. There have been studies, for example, that have concluded that people who primarily stand for long periods of time during the day, instead of lowering their risk for heart disease, maybe up to twice as likely to develop it. Perhaps long periods of standing are not the answer either. It has also been pointed out that standing for extended periods of time isn’t safe for all people, such as those with joint or vascular issues.
However, swapping out some sitting time for standing time is not only about heart disease.
One variable that makes sitting for extended periods damaging to the spine is the sustained contracture of the abdominal and hamstring muscles. This creates an imbalance. This, in turn, creates affecting the mechanics of the lower back. It also increases the load on the lumbar discs.
Using a standing desk, even for a portion of a workday, can minimise this imbalance. This helps maintain better spinal alignment and muscle symmetry.
So is a combination of sitting and standing the answer?
A recent study was performed where office workers of varying ages and body masses used a sit-stand desk where they alternated between sitting and standing throughout an 8-hour workday. The study found that the participants reported a 31.8% reduction in standing desk back pain when compared to sitting for the entire workday.
But just like sitting and leaning forward for extended periods can increase pressure on the back, the same applies to standing with poor ergonomics. Maintaining good posture and taking frequent breaks is the best way to ensure you’re standing or sitting optimally.
Try not to wear high heels (you can swap out for flats or slippers while at your desk if needed). Have the top of the computer screen at about eye level, and vary posture. When you’re in a sitting phase of your day make sure your chair and workstation have been fully ergonomically assessed. Discuss any conditions with your osteopath. They can advise how to adapt both the sitting and standing phases to suit you better. Have regular breaks from your desk altogether when you walk around the office.
And then of course if you really want to blow the budget there are treadmill desks…
If you’re experiencing back pain you can book an appointment with our Osteopath, Andrew Doody, online.
Massages are known to reduce stress and help you relax but they are often overlooked as part of an extensive exercise recovery plan. Not only are they important throughout marathon training programmes but are an essential part of recovery.
Recovering from a marathon is a critical component to a perfect training plan that runners often neglect. Post marathon massages are known to prevent injury, help repair injured muscle tissue and decrease recovery time to help you get back to your training regime quicker. Unfortunately, if you don’t properly recover from a marathon, it will be harder to break your PR and stay healthy.
It doesn’t matter if you’re a professional runner or if it’s your first marathon, the impact of running such a distance has undoubtedly put your body under enormous stress and physical duress.
The most obvious physical impacts are muscle soreness and fatigue which cause damage. It will take your muscles approximately 2 weeks post marathon to return to full strength.
It is essential for marathon runners to have considered a 2-3 week marathon recovery protocol that focuses on rest and rejuvenation and we’d recommend 2 sports massages within that time frame to assist recovery.
It is never recommended to have a massage on the day of a marathon or the day after as your body firstly needs to rest and heal the muscular damage and correct any inflammation.
We’d recommend…
Day 1 – 3 Post Marathon
A light massage or using a roller massage stick to help loosen and stretch your muscles from any delayed muscle soreness. A deep tissue massage isn’t recommended just yet.
Day 4 – 7 Post Marathon
You should consider booking in a deep tissue sports massage. Point out any areas that are really bothering you and use massage to help prevent injuries. Your osteopath can also help identify any injuries you may have and the best action to recovery.
- Effects and benefits of sports massage
- Pumps blood and fluids around the body.
- Helps stretch muscles and improve elasticity.
- Helps get rid of lactic acid build up.
- Breaks down scar tissue.
- Reduces pain.
- Relaxes muscles, body and mind.
- Can help reduce anxiety.
Combining recovery massages with a good diet and plenty of water will help you recover much more quickly.
If you would like to incorporate recovery massages into your marathon training or book in for a post-marathon massage, you can book an osteopathy appointment online. Learn more about our osteopathy services here.
Although fibromyalgia has long existed, it has only recently been accepted as a chronic, debilitating condition.
The NHS and the Department of Work and Pensions now list fibromyalgia as ‘real’, which is a step in the right direction.
So what is fibromyalgia?
The exact cause of fibromyalgia is unknown, but it is thought to be related to abnormal levels of certain chemicals in the brain and changes in the way the central nervous system (brain, spinal cord and nerves) processes pain messages carried around the body.
It may connected to other conditions, including various arthritis’s and may be genetic but even this is unsure. We do know it can be triggered after a traumatic or stressful event; anything from a virus to a divorce. Anyone can develop fibromyalgia at any age, but it predominantly affects women between the ages of 30 and 50. Some studies believe up to 1 in 20 people may be affected.
Symptoms
Unfortunately there is no specific test for fibromyalgia, so diagnosis is made purely on presentation and history. This makes life difficult as the symptoms of fibromyalgia vary according to the person, both in specifics and intensity. Symptoms may be aggravated by many things, from stress to the weather.
Widespread pain
If you have fibromyalgia, one of the main symptoms is likely to be widespread pain. This may be felt throughout your body, but could be worse in particular areas, such as your back or neck. The pain is likely to be continuous, although it may be better or more severe at different times.
The pain could feel like:
- an ache
- a burning sensation
- a sharp, stabbing pain
Extreme sensitivity
Fibromyalgia can make you extremely sensitive to pain all over your body, and you may find that even the slightest touch is painful.
If you hurt yourself – such as stubbing your toe – the pain may continue for much longer than it normally would.
You may hear the condition described in the following medical terms:
- hyperalgesia – when you’re extremely sensitive to pain
- allodynia – when you feel pain from something that shouldn’t be painful at all, such as a very light touch
You may be sensitive to things such as smoke, certain foods and bright lights. Being exposed can cause your other fibromyalgia symptoms to flare up.
Cognitive problems (‘fibro-fog’)
Cognitive problems are issues related to mental processes, such as thinking and learning. If you have fibromyalgia, you may have:
- trouble remembering and learning new things
- problems with attention and concentration
- slowed or confused speech
Other symptoms
Other symptoms that people with fibromyalgia sometimes experience include:
- dizziness and clumsiness
- headaches
- fatigue
- poor sleep quality
- stiffness
- feeling too hot or too cold – this is because you’re not able to regulate your body temperature properly
- restless leg syndrome (an overwhelming urge to move your legs)
- tingling, numbness, prickling or burning sensations in your hands and feet
- in women, unusually painful periods
- IBS developments
- anxiety
- depression
If you think you may be depressed, it’s important to get help from your GP or your fibromyalgia healthcare professional, if you’ve been seeing one.
So what can be done to help?
First and foremost you need a good diagnosis from your heathcare practitioner to make sure they think you have fibromyalgia and not other conditions that may need treating differently, or more importantly investigating differently to be safe.
Once this is done and other conditions have been ruled out, and fibromyalgia has been diagnosed, you may need to try a variety of treatments to find a combination that suits you.
Fibromyalgia has numerous symptoms, meaning that no single treatment will work for all of them. Treatments that work for some people won’t necessarily work for others.
These treatments include medication, lifestyle changes (from diet to identifying and avoiding trigger factors), exercises, physical treatment, relaxation techniques, counselling and CBT.
Article by Andrew Doody – Osteopath for Fleet Street Clinic
There are many helpful bodies out there who can help and support if you are concerned you may suffer from fibromyalgia including UK Fibromyalgia, Fibromyalgia Action UK and the Fibromyalgia Association.
HOW TO BOOK AN APPOINTMENT
You can find more information about out osteopathy services here. Or book an appointment with out osteopath, Andrew Doody.
Arthritis and Osteopathy
Are you living with arthritis or know someone who is? Many people have experience of arthritis – there are currently 10 million people in the UK affected. Sufferers can often resign themselves to living with the pain, without realising there are a number of ways to manage it. For World Arthritis Week, we take a look at arthritis and the benefits of using osteopathy to help treat the condition.
What is arthritis?
Arthritis is a common condition which causes pain, swelling and inflammation in the joints of the body.
The most common types are osteoarthritis and rheumatoid arthritis. Osteoarthritis is a result of wear and tear of the joints in the body. It is common in people over 50 and can affect the knees, hips, neck and back, feet and hands.
Symptoms of Arthritis
Arthritis may be hereditary but can often be caused by poor posture, heavy manual work and previous injury, symptoms include:
- Hip / Knee Pain
- Neck Pain
- Lower back pain
- Early morning stiffness
- Joint Pain
- Swelling and Inflammation
- Referred muscle pain
What can osteopaths do to help with arthritis?
The Institute of Osteopathy purports osteopathy as a way to manage arthritis and the associated symptoms. Mobilising arthritic joints and treating surrounding muscles can help reduce pain. Osteopaths work on the general mobility of the other joints and muscles in the body to improve overall function. Osteopaths may advise on posture, diet, exercise and health improvements.
Osteopaths in Central London
Top Osteopath, Andrew Doody works at Fleet Street Clinic in London and is able to treat arthritic conditions and help to alleviate pain. Osteopathic treatment can be used in conjunction with help from a dietitian, use of acupuncture and support from your GP to ensure a holistic treatment of the condition.