Tag: podiatry
WINTER FEET – LOOKING AFTER YOUR FEET IN COLD WEATHER
ADVICE FROM OUR PODIATRIST, George Hill
Staying warm when it’s cold outside can be a challenge. Especially when it affects our body’s circulation; our feet and hands can suffer especially. In cold weather, it is a natural response to prioritise the heating of our vital organs. This is so they remain at their optimal temperature for full functionality. This means having cold feet is normal when the temperature drops. Nail growth slows down and skin will often become drier because nutrition to these tissues is affected.
In response to this temperature change, small blood vessels temporarily constrict. As a result, you may see a change in the colour of your skin, which could look pale, blanched and waxy at first, before becoming bluish. This is because the oxygen in the blood has been used up by the tissues. The skin is also cool to touch. Returning to warm conditions usually remedies this and the skin becomes pink and warm again.
However, in some individuals, this response is exaggerated and prolonged. This condition is known as Raynaud’s phenomenon and can be inherited. The same response will occur but much more readily and will last longer. Meaning the colour changes are much more obvious. When the skin is deprived of oxygen for long periods of time, some injury occurs to the soft tissues. This can make fingers and toes numb while they remain cold. When the blood vessels do finally relax and blood returns to the area, fingers and toes can throb and burn, turning bright red with inflammation. Eventually, things return to normal but repeated episodes of this can lead to dry, devitalised skin and changes in nail shape and texture.
Chilblains occur for much the same reason. These are painful, itchy swellings that often occur on the tops of small toe joints but can occur in other bony areas too, such as the back of the heel. Tightly fitting footwear can add to the misery by constricting blood flow further and rubbing on the painful skin. Chilblains are not caused by using hot water bottles, as commonly thought, they are a cold injury to Winter Feet, The attempt to relieve the intense itch by scratching merely worsens the problem, often causing further damage. Itching tends to break the skin and causes sores which can sometimes lead to infections.
Preventative action should reduce the likelihood of chilblains developing, but if they do, an antipruritic (anti-itching) cream or ointment can be obtained from pharmacies, and menthol-based products can also be very soothing.
If the skin becomes broken, antiseptic creams such as Savlon help the skin to heal and prevent infection. Cover with a gauze pad after applying, which can be secured with finger bandage or held in place with a cotton sock.
In the aftermath of chilblains, the affected skin is often dry, thin and rough, so use a moisturising cream to restore normal texture.
Cold feet at night can keep you awake or disrupt sleep.
What can be done to help? If you are susceptible to cold extremities, it is important to keep yourself generally warm. Listen to the temperature forecasts and dress accordingly. As well as suitable outer clothing, trousers, tights or socks will help to keep the whole limb warm. Fibres such as wool or bamboo are good insulators and several light layers, rather than one thick layer, traps more air and heat. Remember to wear roomier footwear to allow for thicker socks without compressing the skin.
Footwear should have a good rubber or composite material sole, to insulate against cold pavements – adding insoles of cork or lambswool can improve insulation and comfort. The sole should have good grip for traction on slippery pavements.
Keep active – this improves circulation, and have plenty of hot drinks and food throughout the day.
At home, a warm (not hot) foot-bath will help. Dry with a rough towel and apply a cream or lotion with a massaging action. Some preparations include ingredients such as capsaicin or ginger, to stimulate circulation. Afterwards, put on loosely-fitting, warm socks or slippers to maintain the effect. If the feet are warm before going to bed, they are likely to stay warm. Bed socks in wool or cashmere can be very helpful. Water bottles or gel pads should not be over-heated, as sensation can be unreliable in cold feet.
People who suffer from eczema will find that cold weather tends to make the skin even drier and more cracked. Use plenty of ointment to keep the skin well hydrated and wear hose to help trap moisture and warmth. Silk is a good choice of material and is thin enough to wear under a thicker, outer sock.
In severe cold weather, you may find you get recurrent problems in your feet. Consult your GP who may advise a prescription drug to relax the constricted vessels and thus improve blood flow to the extremities.
Book Your Winter Feet Podiatry Appointment
For more information about podiatry at Fleet Street Clinic
It’s now coming to the end of summer and many of us have spent plenty of time around pools and on the beach. Which can be wonderful, of course. However, bacteria and viruses can thrive in these locations causing foot infections.
George, our podiatrist talks about one in particular: the pesky verruca.
Verrucae are commonly found on the foot and are relatively harmless. However, there is the possibility they have other more sinister properties. Some can become malignant and/ or grow and spread across the foot causing a host of uncomfortable or potentially dangerous problems.
Verruca or Verrucae are caused by the Human Papilloma Virus (HPV). There are hundreds of different types of HPV and different strains infect the body differently. Some types infect the skin, causing verrucae. Even if you come into contact with the virus that causes warts, the risk of becoming infected and developing a wart is small.
Common warts and plantar warts are not usually a serious health concern. These viral warts have not been shown to play an aetiological role in wider known high-risk HPV-linked diseases* such as cervical cancer and Bower’s disease. This is due to HPV presenting as different strains. Having one does not mean you have the other.
*For additional information on HPV’s link to cervical cancer and HPV’s link to Bowen’s disease, we recommend Macmillan’s website.
Contrary to what the old wives tale would have you believe, warts are not caught from touching a toad. Viral plantar warts are in-fact contracted via skin to skin contact or surface to skin contact; among other suggested routes. While common warts are usually painless, plantar warts can be painful because they press inward when you stand on your feet.
In appearance, these lesions are lumps that are generally circular in shape and appear slightly raised and can be callused over with thicker skin. Some will present with small black/deep-red specks, often noted as the capillary heads and others can be clustered into groups. If you have any small areas of skin you are concerned about then it is important to have these reviewed by your Podiatrist immediately.
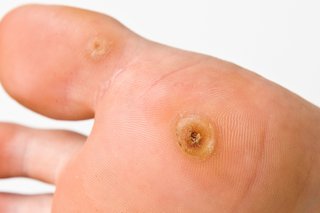
For many, a verruca will disappear in a few weeks to months. However, if they do not it is likely you will require treatment to remove them before they grow or spread. Although one small verruca can be pain-free but unsightly, a large cluster can be quite painful to walk on. Adjusting your walk to relieve the pain can lead to further foot complications. So, it is best to take action as soon as possible.
Over the counter treatment options may work for some people. However, stubborn, persistent verruca will require more appropriate specialist treatment and observation. A medical professional should review all lesions. This is very important so to rule out more serious health concerns.
Specialised treatment is often provided with minimal pain with great results. High strength acid paste or cryotherapy using true liquid nitrogen can be the most appropriate methods for nearly all strains of verrucae. Your podiatrist will advise you on the best course of action based on the verruca presentation, your lifestyle and detailed medical history.
We advised you do not begin treatment without consulting a medical practitioner first. Your Podiatrist should be the first port of call when dealing with these pesky verrucae.
For more information about our podiatry service, our foot health check-up, cryotherapy and medical pedicures.
By George Hill | Podiatrist | September 2019
There is no denying that a marathon is an extraordinarily long distance to run and the effects it has on the body can be enormous.
No part of the body is more affected than your feet.
From the intense training regime to the 26.2 miles of constant pounding on hard concrete, it is crucial you look after your feet before and after the London Marathon.
There are many injuries that can be picked up whilst training such as blisters, callus build-up, cracks in the heal and ingrown toenails. Vigorous long-distance running can amplify these injuries but also cause nail damage and even loss of a toenail.
Caring for your feet post marathon is extremely important and visiting a podiatrist is advised to reduce the possibility of long-term damage which could be irreversible.
The key to post-race recovery starts with putting your feet up, relax them with some rest and then think about booking a podiatrist appointment roughly 3 days after your marathon. This will allow any soft tissue that has become inflamed to reduce.
If you have nail damage:
It is important that any pain caused by nail damage be investigated by a podiatrist, this could be from a loose nail to a build-up of pressure from a blood blister under the nail. Following trauma never force the removal of a nail or attempt ‘home-surgery’ as you are likely to create a nail bed infection and increase the risk of causing more long-term damage – leave this to a podiatrist.
If the nail damage isn’t significant nor causing any pain, you can protect it to reduce any further damage and monitor it’s healing. If the area doesn’t heal or begins to become painful it is advisable to book in with a podiatrist for medical help.
If you have excessive swelling and bruising:
These two symptoms can be a key indicator of a fracture, even in the absence of noticeable pain.
In some cases, adrenaline from running the marathon can conceal the pain caused by the fracture and the runner will push on and either ignore the warning signs or simply not register the pain. If swelling occurs for a prolonged period of time or a new bruise develops up to a couple of days post marathon, it is recommended that you seek advice from a podiatrist or visit a GP.
Post race foot care is an extremely important part of your post-race aftercare and will speed up your recovery time and in turn, will mean you can begin training for your next marathon quicker and with healthy feet.
If you would like to incorporate a podiatry appointment into your marathon training or book in for a post-marathon foot care appointment, you can book an appointment online.
Simple Steps to Summer-Ready Feet
It’s officially the start of summer! Good news for feet – it’s time to swap shoes for lighter footwear and sandals. But before you reveal your toes, give your feet some attention so look and feel their best.
Let’s start with your toenails
- Keep your nails short and well-shaped – use a good-quality file to smooth the edge after cutting them
- Use a little oil (almond oil works wonders!) on dry nails – rub into the surface and the cuticles to improve their texture
- Don’t cut cuticles though, this can lead to infection
- Did you know that nail polish can cause your nails to dry out? From time-to-time, leave off the colour and use oil to recondition them
- If you’ve had an injury or infection, then nail can sometimes thicken or become misshapen, making them difficult or painful to cut. These are best dealt with professionally and Podiatrists have the expertise help you.
Time to think about your skin
Healthy skin should be smooth and supple. Rough, thickened or callous skin, often occurs on areas of the feet which have to work particularly hard and this can be unsightly and uncomfortable. Additionally, your skin can become very dry which causes it to harden and crack, especially around the heels. In the summer, when open shoes or sandals are worn, dryness can become even worse.
Painful callouses can be pared away by a podiatrist who can advise you on how best to care for your skin. There are excellent creams and lotions available to improve your skin’s texture and comfort which, when used regularly, can make a lasting difference.
Some people suffer from skin that sweats excessively, a problem that tends to be made worse in warm weather or after activity and sports. This makes your skin more prone to chafing, blisters and fungal infections (athlete’s foot) and verrucas (plantar warts). Using a good antiperspirant can help with this (eg Dri-clor), as can dusting powders and a better choice of sports socks.
Having lots of small, itchy blisters on your skin, splits between your toes or flaky patches usually means a fungal infection, while verrucas are caused by a viral infection and both need specialist products to treat them. Podiatrists are experts in advising on and treating skin infections.
You can help protect yourself against infections by wearing flip-flops when walking in areas used by many people, by drying your feet thoroughly and by airing sports footwear well after use (fungi love soggy trainers!)
Finally, don’t forget your feet can get sunburned. If you are walking in sandals on a sunny day, remember to apply suncream regularly to the top of your feet.
Don’t forget the right footwear
As with all types of footwear, summer shoes and sandals need to be well-fitting and appropriate for the activities you are doing. Feet get bigger throughout the day, especially in hot weather, so sandals need to be adjustable to allow for this.
Pavement pounding
Flip-flops are beach shoes and are not suitable for day-long wearing on pavements. Your muscles have to work hard to keep these on your feet, so they will be tired and sore by the end of the day. Instead, choose sandals with a thicker, shaped sole, sometimes known as Fit-flops, which are held in place by a strap and give much greater support and cushioning to your foot. This is especially important if you are planning a day’s walking and sight-seeing.
Trekking footwear
Serious trekking requires a well-designed walking shoe – don’t skimp on cheap shoes or socks! You can find these in specialist retailers for outdoor activities.
Now get out there and enjoy the longer days…
Walking is an excellent activity to improve your fitness. It gives benefits to all your bodily systems, strengthens muscles and bones, improves mood and concentration and can help you to lose weight too. Aim to walk at least thirty minutes a day and keep up a brisk pace. If you are visiting the coast, walking barefoot on a sandy beach gives your foot muscles a good workout and helps to keep your feet strong and supple.
Fleet Street Podiatry Clinic
For further advice and information on treatment and how to look after your feet, see our podiatry page. Or you can book an appointment online.
- We have a small, friendly team of specialists, who are all HCPC registered professionals, with a broad range of skills and experience.
- We take a team approach to care: our podiatrists work together with our in-house osteopath, GPs, acupuncturist and dietician to give you the best support for your foot health problems.
- We have an excellent network of trusted colleagues to whom we can refer, with expertise in dermatology, physiotherapy, radiography, sports medicine and surgery.
- We will look after your foot-health at a time convenient to you – day and evening appointments always available!
- We stock a range of professional foot-care products to help you to get the best out of self-care between appointments.
Book your Podiatry appointment today. Or find out more about our podiatry clinic here.